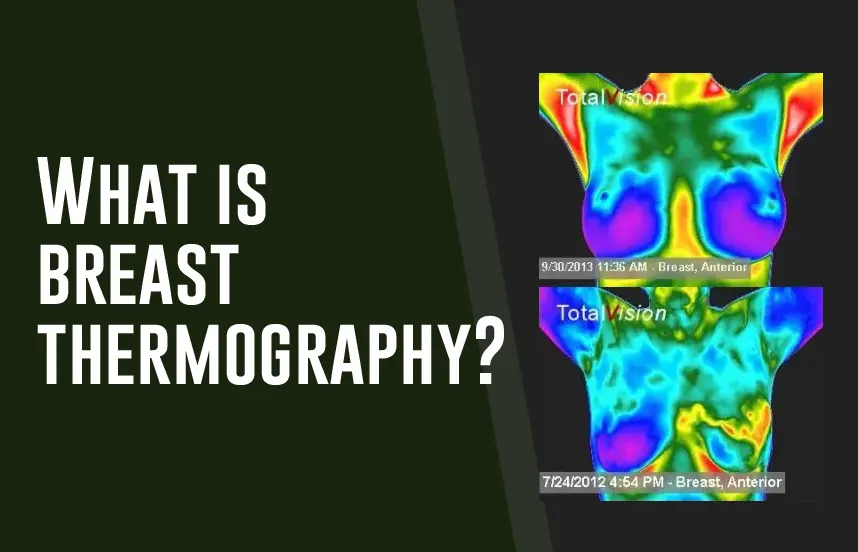
Breast thermography is an imaging technique used to detect breast cancer in women. It is a non-invasive and radiation-free procedure that uses infrared technology to measure breast temperature. It has the potential to detect breast cancer at its earliest stages when it’s much easier to treat and has a better chance of successful treatment.
The breast thermography process begins with the patient lying on their back in a darkened room. Illuminating their breast area with an infrared camera. This camera captures images of the breast tissue and records the amount of heat emitted from each area. A computer interprets these signals and produces a detailed report indicating abnormal findings or breast abnormalities. Using the information from breast thermography determines whether further tests are necessary.
The accuracy of breast thermography depends on several factors. Including the quality of the equipment, the experience of the technician performing the procedure, and the size and shape of the breasts. Breast thermography results may be slightly more accurate for larger breasts than for smaller ones. It is because larger breasts produce more heat than smaller ones. Additionally, breast density can affect results. Dense breast tissue may produce false positives. The heat it emits from dense areas may mislead as indications of cancerous changes. In comparison, normal breast tissue can appear more relaxed than expected.
Breast thermography offers several advantages compared to other breast cancer screening methods, such as mammograms. It does not use radiation or involve mechanical compression, which can be uncomfortable for some patients. In addition, breast thermography can often detect temperature changes. Before, other traditional testing methods could pick up any signs or symptoms related to breast cancer. Furthermore, this imaging method is less expensive than other screening techniques. It provides results much faster than traditional methods like mammograms. Which usually takes two weeks or longer to complete.
Despite its potential benefits, some downsides are associated with breast thermography. For instance, it is not recommended as a replacement for mammogram screenings; instead, it should be used alongside mammograms to accurately diagnose potential problems in time for early detection and treatment if needed. Additionally, since this method relies on measuring temperature changes to conclude a woman’s health condition, accuracy could suffer if body temperatures vary too widely due to various external factors such as exercise or fevers occurring during measurement times.
Lastly, some studies have suggested that this type of imaging may produce false positive results due to certain environmental factors that impact skin temperatures, such as air conditioning systems or hot weather conditions. It affects readings taken over certain timespans. It leads to inaccurate conclusions by technicians analyzing the test results. Obtained via thermal imaging devices used during procedures involving this type of technology.
In conclusion, even though there are drawbacks to using breast thermography for medical purposes, it still offers a reliable alternative method for detecting signs and symptoms related to possible cases of early-stage breast cancer. Prevention is better before they become too severe or complicated to treat appropriately.
This imaging technique has dramatically improved over time, resulting in greater accuracy levels when performed by qualified professionals. Meaning that more patients have access to safer treatments earlier on, helping them recover more quickly from their diseases without having gone through invasive procedures, which pose added risks even if only performed on a preventative basis. Doing so provides peace of mind for those undergoing a course these tests, which hopefully leads them closer to achieving total recovery rates soonest possible.


